Vertebral Compression Fractures in Osteoporosis: Diagnostic Imaging Tips
Vertebral compression fractures (VCFs) are commonly discovered incidentally in primary care. They often appear on imaging ordered for unrelated reasons, e.g., back pain, chest imaging, abdominal CTs, or trauma workups.
The key point: a vertebral compression fracture in adults >50 is usually a fragility fracture, which automatically signals high future fracture risk and should prompt an osteoporosis assessment and treatment discussion (1).
Because these fractures are not always highlighted in radiology conclusions, it is helpful for primary care clinicians to recognize the common imaging clues.
First, we’ll recap what osteoporosis is, how to assess for a VCF, and some diagnostic imaging pearls for spotting a VCF.
What Is Osteoporosis?
Osteoporosis can be diagnosed in 3 ways:
1. DEXA T-score ≤ –2.5
Osteopenia: –1.0 to –2.4
2. Fragility fracture after age 40 (in patients >50).
Osteoporotic fractures (fragility fractures, low-trauma fractures) are those occurring from a fall from standing height or less, without major trauma such as a motor vehicle accident. Vertebral compression fractures are the most common type of osteoporotic fracture.
This includes fractures of the:
Hip
Vertebral
Humerus
Pelvis
Excludes fractures of the:
Hands
Feet
Craniofacial fractures
3. 10-year major osteoporotic fracture risk ≥20% (FRAX or CAROC) (2)
Why Catching Vertebral Compression Fractures Matters
Fractures lead to:
Increased morbidity
Excess mortality
Loss of independence
Reduced quality of life (2)
We want to pay special attention to vertebral compression fractures — how to spot them clinically or on diagnostic imaging. Let’s run through three common scenarios in which VCFs can be detected.
Scenario 1: Clinical Manifestations of a Vertebral Compression Fracture
Clinical assessment for a hidden VCF should be done in all adults over the age of 50.
Major risk factors for an undiagnosed vertebral compression fracture (VCF) includes:
Previous fracture after age 40
Glucocorticoid use >3 months (≥5 mg prednisone daily)
≥2 falls in the past year
Parental hip fracture
BMI <20
Current smoker
≥3 alcoholic drinks daily
Secondary causes
Signs of an occult VCF on exam:
Height loss >2 cm recently or >6 cm historically
Rib-to-pelvis distance <2 fingerbreadths
Occiput-to-wall distance >5 cm (1)
Assess for:
Falls
new onset or chronic back pain
Limitations in physical functioning and activities of daily living (1)
Rule out red flags:
Dermatomal sensory deficits
Focal weakness
Upper motor neuron signs (e.g., clonus)
Neurologic abnormalities may indicate retropulsed bone fragments in the spinal canal or foramina, which may require surgical intervention. In such patients, urgent imaging with magnetic resonance imaging (MRI) or computed tomography (CT) and prompt consultation with a spine surgeon should be obtained (1).
👉 Practical tip: Measure height at every annual visit in adults >50.
If you suspect a VCF clinically, diagnostic imaging is recommended, starting with plain radiographs of the thoracolumbar spine (1,3). Choosing XR versus CT may depend on the patient’s presentation (e.g., severity of symptoms or ability to stand/position for imaging) (3. Plain radiographs are a reasonable initial option for patients with mild-to-moderate pain who can tolerate standing and have no evidence of fracture-related complications (1).
💡 Bottom line: Osteoporosis can be diagnosed with DEXA scan T-scores, if a fragility fracture has occurred, or if fracture risk (using validated tools like FRAX) is >20%.
Scenario 2: Fragility Fracture With No Prior Diagnosis
If a patient presents with a suspected fragility fracture clinically and it is identified on imaging (hip, vertebral, humerus, or pelvis fracture), they are automatically considered high risk for future fractures, regardless of fracture risk score or BMD.
Plan: Order a DEXA scan for baseline (if not already completed) → initiate treatment to reduce fracture risk (high risk for fracture = highest benefit for pharmacologic treatment).
Scenario 3: Incidental Vertebral Compression Fracture
An incidental VCF on imaging ordered for another purpose (e.g., plain radiographs or CT scans) is common in adults >50. These findings are treated as a fragility fracture and indicate high risk for future fractures. It’s important to recognize VCF imaging findings, as they are not always explicitly labeled as such on the radiology report.
Plan: Order a DEXA scan for baseline (if not already completed) → initiate treatment to reduce fracture risk (high risk for fracture = highest benefit for pharmacologic treatment).
💡 Bottom line: An incidental vertebral compression fracture in adults >50 is considered a fragility fracture and automatically places the patient at high risk for future fractures, regardless of BMD result or FRAX/CAROC score. Initiate appropriate pharmacologic and non-pharmacologic therapy.
Diagnostic Imaging: X-Ray Clues for Vertebral Compression Fractures
Let’s familiarize ourselves with common VCF findings and the test characteristics of plain radiographs - this is important as the radiology report conclusion will not always include a diagnostic label of a VCF.
Radiograph Clues for Vertebral Compression Fractures
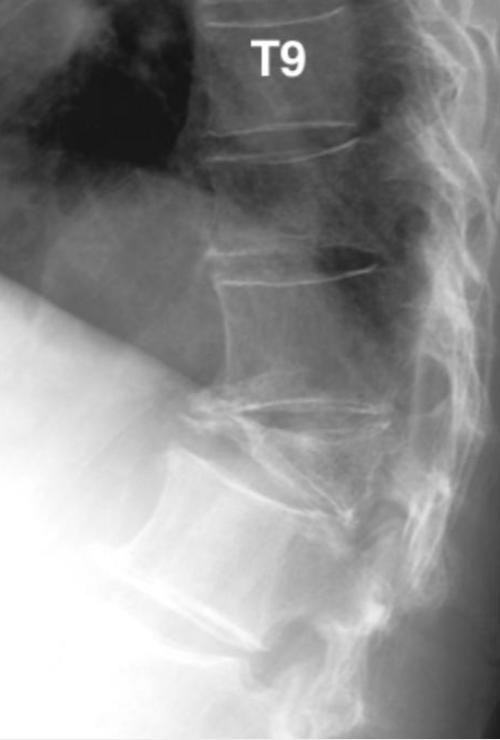
Anterior wedging: the classic finding, where the front of the vertebral body collapses while the back remains relatively intact, resulting in a wedge-shaped vertebra
≥20% height loss or >4 mm reduction from baseline
Increased radiodensity: the fractured bone often appears whiter on the X-ray due to compaction of trabecular bone
Cortical step-off: disruption in the normal smooth, rectangular outline of the vertebra
Kyphotic deformity: severe cases or multiple fractures can cause the spine to curve forward, creating a “round back” or “dowager’s hump” (4,5).
Kümmell disease involving the T10 vertebral body with an osteoporotic spinal compression fracture at T12 - wedge shape deformity (5).
How to Differentiate Acute vs Chronic Vertebral Compression Fractures
Acute fractures: Often show clear cortical disruption, a distinct fracture line, and sharp angulation.
Chronic fractures: Typically show permanent height loss without evidence of a new fracture line, along with degenerative changes such as surrounding osteophytes (4,5).
Test Characteristics of Plain Radiograph for Vertebral Compression Fractures
Plain radiographs miss approximately two-thirds of vertebral compression fractures. X-ray has especially low sensitivity for minor fractures (compared with severe ones). This means that if the results are “normal” but clinical suspicion remains high, CT may be the next step, as it is superior for examining bony anatomy.
Plain radiographs also cannot always differentiate acute versus chronic fractures, so results should be interpreted in the clinical context (recent trauma, no recent trauma, gradual height loss, etc.) (4,5).
💡 Bottom line: Plain radiographs can miss minor fractures and cannot always differentiate acute versus chronic VCFs. If you still have a high index of suspicion for a VCF despite a normal radiograph, a CT of the spine is a reasonable next step.
Top Takeaways:
Vertebral compression fractures (VCFs) are often under-recognized but clinically important. In adults >50, a VCF is usually a fragility fracture, signaling high future fracture risk and the need for osteoporosis assessment and treatment—even if discovered incidentally on imaging.
Clinical suspicion is key and relies on risk factors, history, and physical exam. Look for recent height loss, back pain post-fall, limited function, or high-risk features (previous fracture, glucocorticoid use, falls, low BMI, smoking, alcohol). Red flags (neurologic deficits) require urgent imaging and referral.
Diagnostic imaging has limitations, but certain X-ray findings are clues. Plain radiographs may miss minor fractures and cannot always differentiate acute vs chronic VCFs. Look for anterior wedging, height loss, cortical step-off, increased radiodensity, and kyphotic deformity. CT can be used if suspicion remains despite normal X-rays.
💡For weekly diagnostic imaging insights and practice-changing pearls, join NP Reasoning Masterclass.
ReferencesRosen HN, Hirsch JA. Osteoporotic thoracolumbar vertebral compression fractures: clinical manifestations and treatment. In: Rosen CJ, editor. UpToDate. Waltham (MA): UpToDate Inc.; 2026. Available from: https://www.uptodate.com/contents/osteoporotic-thoracolumbar-vertebral-compression-fractures-clinical-manifestations-and-treatmentMorin SN, Feldman S, Funnell L, Giangregorio L, Kim S, McDonald-Blumer H, et al. Clinical practice guideline for management of osteoporosis and fracture prevention in Canada: 2023 update. CMAJ. 2023;195(39):E1333–48. doi:10.1503/cmaj.221647.Canadian Association of Radiologists. CAR spine referral guideline. Ottawa (ON): Canadian Association of Radiologists; 2024. Available from: https://car.ca/wp-content/uploads/2025/03/CAR_Spine_Referral_Guideline_FINAL.pdfMitchell RM, Jewell P, Javaid MK, McKean D, Ostlere SJ. Reporting of vertebral fragility fractures: can radiologists help reduce the number of hip fractures? Arch Osteoporos. 2017;12(1):71. doi:10.1007/s11657-017-0363-y.Bashir U, Walizai T, Elfeky M, et al. Spinal compression fracture. Radiopaedia.org. Available from: https://doi.org/10.53347/rID-19197. Accessed 2026 Mar 5.